Glaucoma

Why Come to Florida Eye for Glaucoma Treatment?
In any given year, physicians at Florida Eye Microsurgical Institute perform numerous glaucoma-related eye exams and procedures. Glaucoma is the second leading cause of blindness in America, and the doctors and staff at Florida Eye understand the importance of annual eye exams, especially for those at risk of the disease. Our doctors will help you determine the best course of glaucoma treatment for your particular condition. Should you be on medication or are you a candidate for Selective Laser Trabeculoplasty (SLT), a surgery for glaucoma? We will help you make that decision.
Why Choose a Florida Eye Doctor to Treat Your Glaucoma?
We have exceptional doctors who are equally caring, skilled and available at Florida Eye. Dr. Schechter mainly practices at our Boynton Beach location and is available one day in our Boca Raton practice.
Learning I did indeed have glaucoma was not pleasant, to say the least, but you were so kind and reassuring to me that I was able to put my concerns to rest. I am so very glad I was diagnosed early, and I will certainly be compliant with your instructions.
Most appreciatively, Earl
Treatment for Glaucoma
If you’ve been diagnosed with glaucoma, prompt treatment is essential to preventing further vision loss and optic nerve damage. While there is no cure for glaucoma, there are many options available to help stabilize the condition or stop it from progressing.
Your eye doctor at Florida Eye Microsurgical Institute will recommend treatment options depending on the severity and progression of your glaucoma, including:

Eye Drops
The most common treatment for glaucoma is often prescription eye drops that help reduce intraocular pressure. Some work by helping fluid flow through the eye’s drainage canal, while others reduce the amount of fluid the eye produces.
If you opt for eye drops to treat your glaucoma, you will need to use the eye drops consistently to safely maintain a healthy intraocular pressure. Unless you elect to receive an implant or procedure for glaucoma, you will likely need to continue using the eye drops for the rest of your life.
Selective Laser Trabeculoplasty (SLT)
Selective laser trabeculoplasty is an in-office laser procedure that uses targeted pulses of low-energy laser light to stimulate the melanin-containing cells within the eye’s natural internal drainage system. This improves fluid drainage through the trabecular meshwork of the eye and lowers intraocular pressure.
When used as a first-line treatment for glaucoma and ocular hypertension, the LiGHT trial found that SLT significantly reduced intraocular pressure, while also reducing the likelihood of needing additional glaucoma surgeries in the future.
Durysta
Durysta is the first FDA-approved biodegradable implant that releases medication (Bimatoprost) to lower the intraocular pressure. If you struggle to use eyedrops consistently or have bothersome side effects from drops, Durysta may be the treatment for you.
It is a microscopic implant that is inserted into the front chamber of the eye and continuously releases Bimatoprost. Although the implant degrades over the course of 6 months, some studies have found that the pressure-lowering effects can last for up to 2 years in some patients.
Laser Surgery
Your eye doctor may recommend one of several other laser treatments offered at Florida Eye Microsurgical Institute, which include:
Laser Peripheral Iridotomy (LPI)
Laser peripheral iridotomy involves creating a small hole in the iris to improve fluid drainage in patients with narrow-angle or angle-closure glaucoma.
Cyclophotocoagulation
Cyclophotocoagulation, or CPC, is a laser procedure that alters the ciliary body, the structure that produces fluid inside the eye. By decreasing how much fluid is produced in the eye, cyclophotocoagulation can reduce the intraocular pressure.
Micropulse Transscleral Laser Therapy
Micropulse is a laser procedure that helps to lower intraocular pressure by improving the drainage outflow of the eye and decreasing the production of fluid within the eye.
Glaucoma Surgery
In some cases, patients with glaucoma may require surgery to lower intraocular pressure. Florida Eye Microsurgical Institute offers both traditional glaucoma surgeries and minimally invasive glaucoma surgeries.
Often called MIGS, these procedures tend to have faster recoveries and take less time than traditional glaucoma procedures. Some of them include:
iStent
iStent is a microscopic stent that can be implanted into the eye’s natural internal drain. This can improve drainage in the front of your eye and lower eye pressure.
Goniotomy
Goniotomy is a procedure that involves removing the first layer of the trabecular meshwork of the eye to improve drainage and reduce intraocular pressure.
XEN Stent
The XEN Gel Stent is a tiny tube implant that allows fluid to drain from inside your eye to a small “bleb” underneath the white part of your eye. Traditional glaucoma surgeries offered at Florida Eye Microsurgical Institute include:
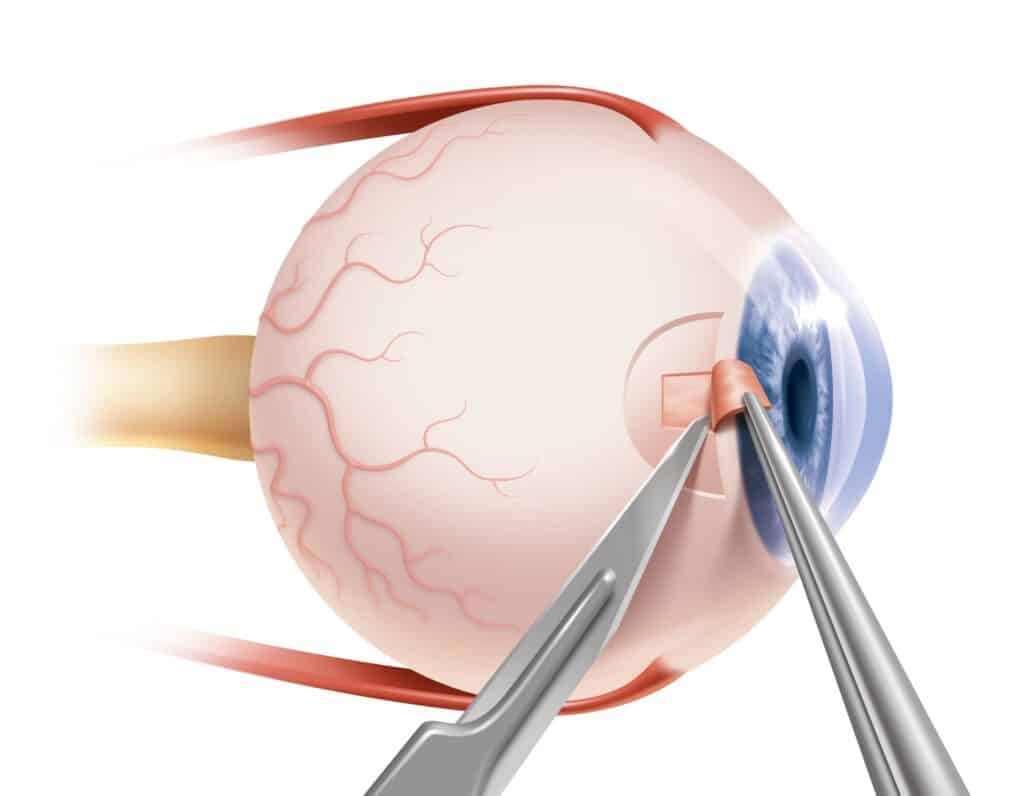
Trabeculectomy
When more minimally invasive options have not effectively managed glaucoma, your eye doctor may recommend a trabeculectomy. During the procedure, they will create a small passageway from the inside to the outside of your eye.
This helps regulate intraocular pressure by promoting fluid flow out of the front of the eye.
Tube Shunts
A thin, flexible tube (a shunt) with a silicone pouch is inserted in the eye to facilitate drainage.
Do you want to learn more about glaucoma treatments and discover whether they could help lower your intraocular pressure? Schedule an appointment at Florida Eye Microsurgical Institute in Boca Raton, FL, today!




